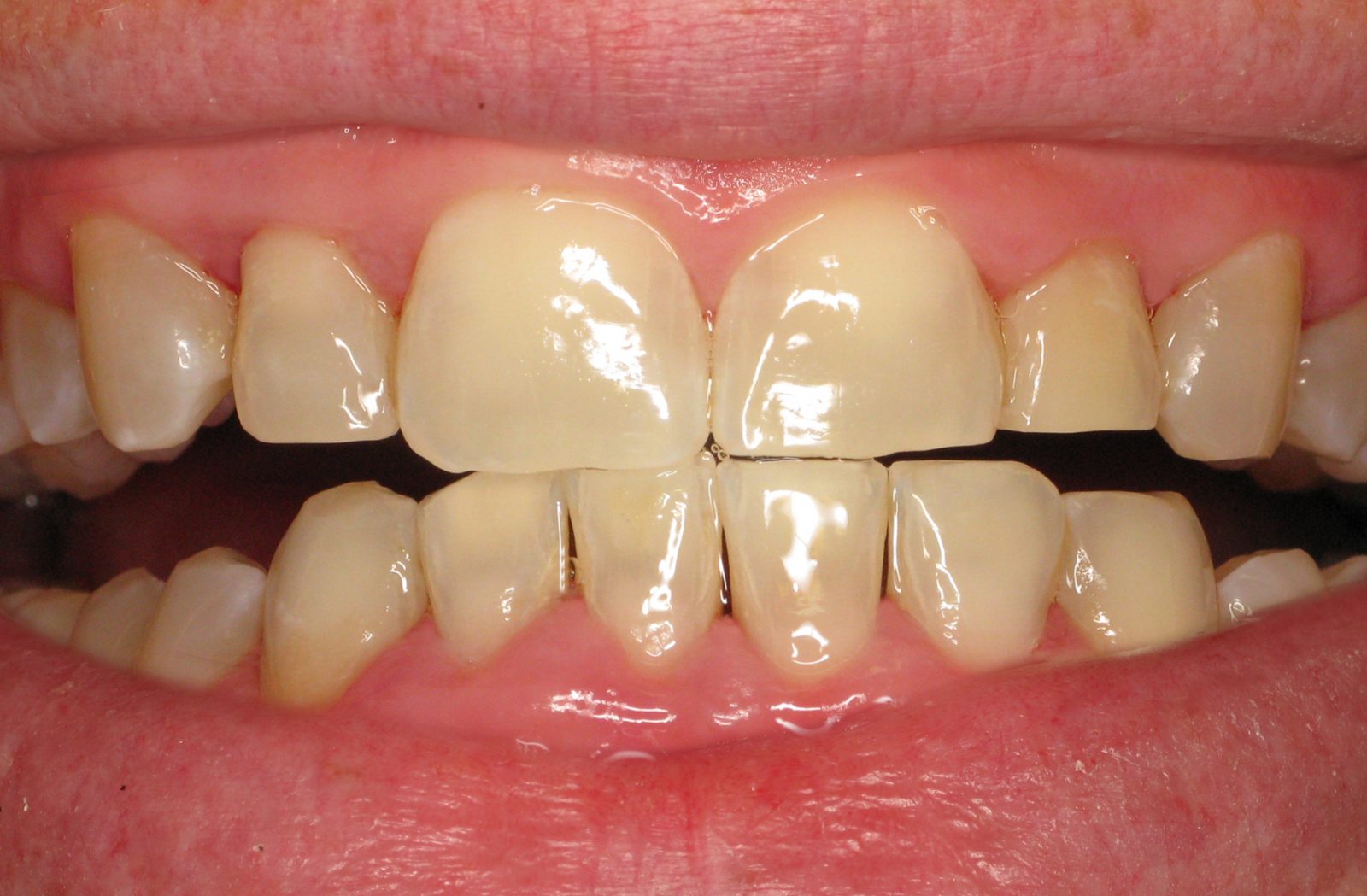
Gum Disease Symptoms: Bleeding Gums

Bleeding gums are a common and often alarming symptom of gum disease, signaling an underlying issue that requires attention. Healthy gums should not bleed during routine activities such as brushing or flossing, but when they do, it is typically an indication of gingivitis, the early stage of gum disease. The leading cause of bleeding gums is the accumulation of bacterial plaque along the gumline. Plaque, if not adequately removed through regular oral hygiene practices, can irritate and inflame the gums, making them more susceptible to bleeding.
As gum disease progresses, the severity of bleeding may increase, potentially leading to further complications. Understanding the causes and addressing bleeding gums promptly through professional dental care and improved oral hygiene practices is crucial for preventing the progression of gum disease and maintaining optimal oral health.
Does Gum Disease cause bleeding Gums?
Gum disease causes bleeding gums primarily due to the inflammatory response triggered by bacterial plaque along the gumline. Here’s a breakdown of how gum disease leads to bleeding gums:
- Formation of Plaque: The process begins with forming plaque—a sticky, colorless film of bacteria—on the teeth. When oral hygiene practices, such as brushing and flossing, are insufficient, plaque accumulates along the gumline and between the teeth.
- Bacterial Irritation: The bacteria in plaque release toxins that irritate and inflame the delicate gum tissues. This irritation is the body’s response to harmful microorganisms, potentially threatening oral health.
- Gingivitis Development: The initial stage of gum disease is known as gingivitis. As the gums become inflamed, they may appear swollen, and red, and, notably, they become more prone to bleeding, especially during activities such as brushing, flossing, or eating.
- Weakening of Blood Vessels: Chronic inflammation in the gum tissues weakens the gums’ tiny blood vessels (capillaries). As a result, these blood vessels are more likely to rupture, leading to bleeding.
- Increased Sensitivity: Inflamed and bleeding gums are often more sensitive, making them susceptible to bleeding even with minimal stimulation. This heightened sensitivity is a key indicator of gingivitis.
- Progression to Periodontitis: gingivitis can progress to periodontitis, a more severe form of gum disease, if left untreated. In periodontitis, the inflammation extends deeper, affecting the supporting structures of the teeth, including the bone. This exacerbates the risk of bleeding gums and can lead to more serious oral health complications.
Regular dental check-ups, thorough oral hygiene practices, and professional cleanings are essential in preventing and managing gum disease. By addressing the root cause of bleeding gums—bacterial plaque—individuals can effectively maintain gum health and reduce the risk of complications associated with gum disease. Call (877) 440-3564 to schedule a consultation with our Laser Periodontics & Gum Surgery specialists to help assess your dental needs.
Why Do Gums Bleed During Gum Disease?
Gums bleed during gum disease due to a complex interplay of factors involving bacterial activity and the body’s immune response. The initial stage of gum disease, known as gingivitis, is characterized by the accumulation of bacterial plaque along the gumline. Plaque harbors harmful bacteria that release toxins, triggering an inflammatory response in the gums. This inflammation leads to a condition known as gingivitis, where the gums become swollen, red, and, notably, prone to bleeding.
The constant presence of plaque and the ensuing inflammation compromise the integrity of the delicate blood vessels within the gum tissues. Weakened blood vessels are more likely to rupture, resulting in bleeding, especially during routine activities like brushing or flossing. This bleeding is an early warning sign of gum disease and underscores the need for timely intervention to prevent the progression to more severe forms of periodontal disease.
Additionally, the bleeding may be exacerbated by factors such as hormonal changes, systemic illnesses, or certain medications, emphasizing the multifactorial nature of gum disease and the importance of personalized care for optimal oral health.
What Role Does Plaque and Tartar Buildup Play in Bleeding Gums?
Plaque and tartar buildup play a pivotal role in the occurrence of bleeding gums, particularly in the context of gum disease. Plaque, a biofilm consisting of bacteria, forms naturally on teeth surfaces. When oral hygiene practices are inadequate, plaque accumulates along the gumline. The bacteria within the plaque release toxins that irritate the delicate gum tissues, prompting an inflammatory response.
As plaque accumulates, it can mineralize and harden into tartar (also known as calculus). Unlike plaque, tartar cannot be removed through regular brushing and flossing. Tartar buildup along the gumline exacerbates the inflammatory process, leading to gingivitis—the initial stage of gum disease.
The presence of both plaque and tartar creates a hostile environment that weakens the integrity of the blood vessels within the gums. Weakened blood vessels are more prone to rupturing, resulting in bleeding gums, especially during activities like brushing or flossing.
Furthermore, chronic irritation from plaque and tartar can develop deep periodontal pockets between the gums and teeth. These pockets become ideal spaces for bacteria to thrive, perpetuating the cycle of inflammation and increasing the risk of bleeding.
Are there other Contributing Factors Leading to Bleeding Gums?
While plaque and tartar buildup are primary contributors to bleeding gums, several other factors can exacerbate this symptom or contribute to its occurrence. These contributing factors include:
- Poor Oral Hygiene: Inadequate or inconsistent oral hygiene practices, such as irregular brushing and flossing, can allow plaque to accumulate, leading to gum irritation and bleeding.
- Hormonal Changes: Hormonal fluctuations, such as those occurring during pregnancy, menstruation, or menopause, can affect gum health and increase the likelihood of bleeding gums.
- Systemic Diseases: Certain systemic diseases, such as diabetes or blood clotting disorders, may compromise the body’s ability to heal and maintain healthy gums, making them more susceptible to bleeding.
- Medications: Some medications, such as anticoagulants or certain antihypertensive drugs, can increase bleeding gums as a side effect.
- Vitamin Deficiencies: Insufficient intake of essential vitamins like vitamin C, which plays a crucial role in gum health, can weaken blood vessels and increase gum sensitivity.
- Tobacco Use: Smoking or tobacco use can hinder the body’s ability to fight infection and impair gum healing, making gums more prone to bleeding.
- Stress: Chronic stress may weaken the immune system and exacerbate inflammation, potentially contributing to bleeding gums.
- Ill-fitting Dental Appliances: Poorly fitting dentures or orthodontic appliances can irritate and contribute to gum bleeding.
- Genetic Predisposition: Some individuals may be genetically predisposed to gum disease and bleeding gums, making regular dental care even more crucial.
- Age: Aging can change oral health; older individuals may experience increased gum sensitivity and a higher risk of bleeding.
Understanding these contributing factors helps individuals and healthcare professionals tailor interventions to address the root causes of bleeding gums. Regular dental check-ups, adopting a consistent oral hygiene routine, and addressing underlying health conditions contribute to maintaining healthy gums and preventing complications associated with gum disease.