Antibiotic Therapy In Periodontics and Gum Disease
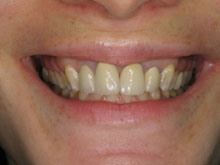
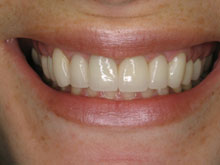
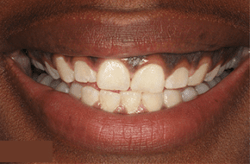
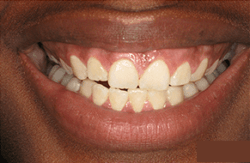
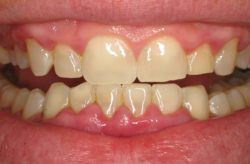
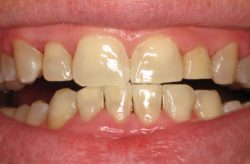
Although gum disease is a common diagnosis, it isn’t easy knowing you have it. When plaque accumulates, it can lead to gum infection, which can cause gum disease. Fortunately, there are effective treatments for gum disease.
Systemic antibiotic therapy in periodontics aims to supplement periodontal treatment such as scaling and root planing with the addition of antibiotics to control the infection by killing periodontal pathogens that survive the periodontal treatment.
Let us discuss some of the most effective treatment options for fighting periodontal disease. We will also highlight the common side effects of system antibiotics.
Rational Antimicrobial Therapy
Rational antimicrobial therapy is an oral medication used to treat bacterial mouth infections. This treatment is intended to prevent and treat gum disease – also known as periodontal disease – and in more severe cases, help with the treatment of periodontal abscesses.
Antimicrobial therapy typically starts with a thorough oral cleaning that includes scaling and root planing. This procedure removes plaque buildup from pockets in the gums. These pockets in your gums are usually teeming with bacteria and would need to be properly cleaned to ensure the antimicrobial treatments are effective.
Following the cleaning procedure, our specialists will prescribe antimicrobial treatment. The most commonly prescribed antimicrobial treatment is antiseptic mouthwash. These mouthwashes contain antibiotics such as Chlorhexidine and Triclosan, which help kill any bacteria forming on the gums and teeth.
Depending on the severity of your case, you should use this mouthwash for seven to ten days.
Antibiotics can also be taken orally, either in pill form – such as Metronidazole for periodontal disease – or applied topically. In severe cases of periodontal disease, antibiotics such as Doxycycline or Minocycline will be directly applied to the gum tissue in gel form.
Furthermore, our specialists may prescribe oral antibiotics and an antiseptic mouthwash to ensure that antimicrobial therapy is effective.
How To Choose Antibiotic Treatment
The most effective way to choose the correct antibiotic treatment is to identify the bacteria you are trying to fight. Undergoing tests such as salivary testing or culture and sensitivity testing will reveal the specific bacteria responsible for your gum disease.
These tests will ensure the most effective antibiotics to treat the condition. With bacterial identification tests, you can be confident you are using the proper antibiotic treatment to treat your particular case of the periodontal disease quickly.
The Common Side Effects Following Systemic Antibiotics
Most systemic antibiotics in periodontal therapy are safe when used correctly. However, systemic antibiotics may cause some side effects. Our specialists typically inquire about allergies to medications before prescribing antibiotics.
Furthermore, an increase in bacterial resistance is another common side effect of systemic antibiotics. Frequent use of antibiotics can lead to causative bacteria building more resistance. As a result, the antibiotics will become less effective. Other common side effects of antibiotics include:
- Diarrhea
- Upset stomach
- Nausea
- Loss of appetite
If you experience any side effects after using systemic antibiotics, we suggest contacting your specialist.
Systemic antibiotics in the treatment of periodontal disease should be used sparingly and supplement non-surgical periodontal therapy. If you suffer from gum disease, consult with one of our experienced specialists to ensure you receive the quality, personalized dental care you deserve.
FAQ
-
What is the best antibiotic for periodontal disease?
There is currently no single antibiotic that is effective against every case of periodontal bacteria and periodontal disease. However, the most common drugs used in periodontal therapy include:
- Amoxicillin
- Clindamycin
- Ciprofloxacin
- Tetracyclines
- Metronidazole
These medications are common local antibiotics for periodontal disease and are often used as scaling and root planing antibiotics.
-
What is the mechanism of action for systemic antibiotics on periodontal conditions?
Antibiotics block biochemical pathways for bacteria. Bacteria typically build a cell wall to protect themselves. The growing bacteria cannot form cell walls. Systemic antibiotics inhibit the biochemical processes that produce the cell wall.
-
How are systemic antimicrobials used in oral healthcare?
Systemic antimicrobials are used to supplement procedures such as scaling and root planing to treat periodontal disease. It is a non-surgical approach to treating and managing periodontitis.
-
How are systemic antibiotics given?
Generally, specialists prescribe systemic antibiotics that can be applied topically or taken orally as pills to help fight the bacteria trapped in periodontal pockets. Furthermore, antibiotics in periodontal therapy: advantages and disadvantages include eliminating certain bacteria and inhibiting the recurrence of periodontal disease. On the other hand, antibiotics may come with some side effects.